A new NHS competence framework for EMDR

Oenone Dudley summarises a new competence framework for EMDR, which she co-authored. The framework was recently published by UCL.
This competence framwork was commissioned by Health Education England (HEE) for the delivery of EMDR for PTSD in IAPT (Improving Access to Psychological Therapies) primary care services. Although the focus of HEE commissioning was for PTSD, the framework also includes the application of EMDR for trauma in the context of other mental health presentations and complex PTSD, in recognition of the fact that EMDR has developed a broader applicability for trauma-based psychological problems that do not necessarily meet criteria for PTSD. The framework is also suitable therefore for secondary care as well as primary care psychological services. Since the inception of IAPT, Roth & Pilling have produced a number of similar competence frameworks covering different modalities of therapy and various clinical populations. They form the basis for assuring the delivery of high quality, evidence-based therapies and for identifying training and supervision needs to assist managers in developing their services. The first was for CBT in 2007. The full suite of competence frameworks can be found here: https://www.ucl.ac.uk/CORE/competence-frameworks
The development of all UCL competence frameworks is undertaken in collaboration with an expert reference group. The expert reference group comprised a service user, Hannah Moore, and senior trainers and consultants: Maeve Crowley, Derek Farrell, Robin Logie, Sandi Richman and Matt Wesson.
It is important to note that the framework produced by UCL is not a substitute for the competency-based accreditation standards that have been developed by EMDR UK. The UCL competence framework has a different remit, situating the skills required to be an EMDR therapist within other generic competences required to practise professionally, ethically and safely. It is also designed to be read by managers and commissioners who are not familiar with EMDR therapy. The skills required therefore are broken down into more detailed descriptions to make them clear and understandable to people who are not familiar with the language of EMDR therapy. In this sense, it is broader and more extensive than the EMDR UK accreditation standards and geared towards wider NHS service development and clinical governance. It is not a framework for accreditation. Neither does it prescribe what service managers should do but it can be used by managers and commissioners to identify gaps in provision, training and supervision and provide a basis for planning and developing services to meet local need.
Six domains
The breadth of the framework is illustrated by the fact that it includes generic as well as EMDR-specific competences required to deliver good therapy (Figure 1). There are six domains which describe each set of skills.
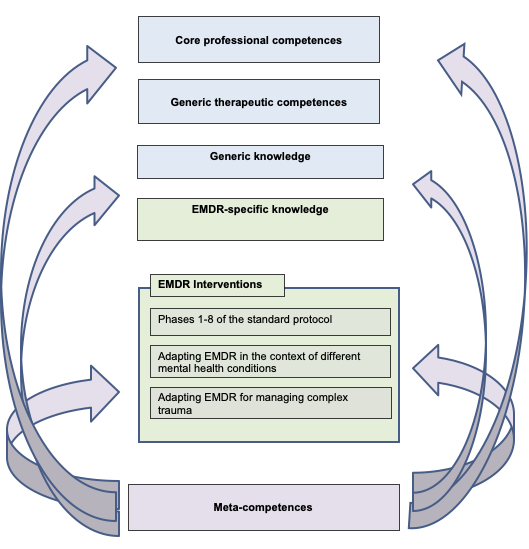
Figure 1: Outline model for the framework
These are:
- Core professional competences, for example working within ethical and professional guidelines; knowledge of capacity, confidentiality and consent; cultural sensitivity and respect for diversity; and use of supervision
- Generic therapeutic competences that are not specific to EMDR, for example knowledge of different therapeutic models; knowledge of mental health problems, generic assessment skills, fostering a therapeutic relationship, responding to distress, managing endings, engagement, using outcome measures, assessing and managing risk, and safeguarding
- Generic knowledge of trauma, for example knowledge of symptoms of PTSD, trauma and dissociation
- EMDR- specific knowledge, in other words the AIP model
- EMDR interventions, which cover the eight phases of EMDR and adaptations that may be required for delivering EMDR for trauma in the context of other presentations, including complex PTSD
- Meta-competences, which describe the skills required to make decisions about how, why and when to implement any assessment or intervention
An interactive map covering the six domains and the constituent competences is available on the website (Figure 2). This enables you to select any domain to identify the set of competences for that domain.
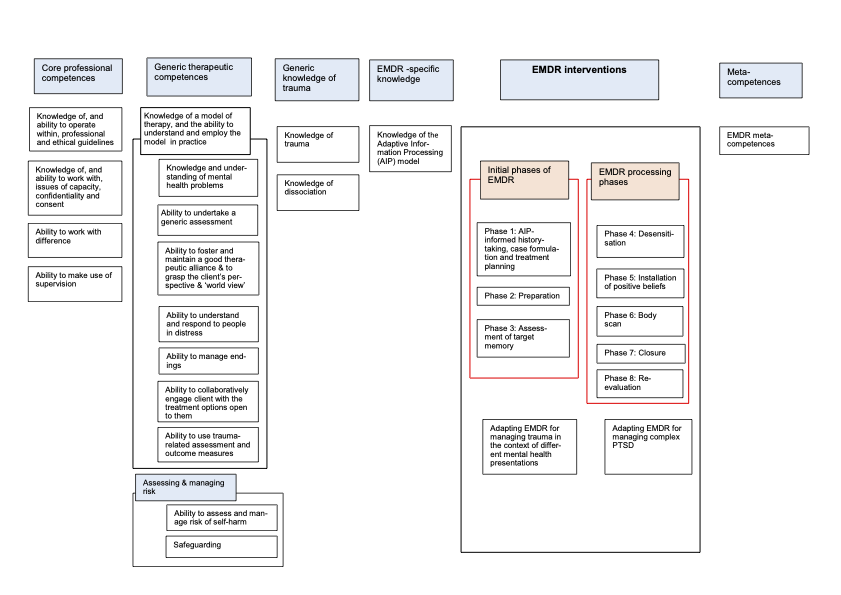
Figure 2: An interactive map covering the six domains and the constituent
competences is available on the website
The framework is accompanied by a supporting document describing the background and rationale and a service user leaflet explaining the experience of EMDR therapy in simple language.
How might the framework be used?
Commissioning EMDR training
The Framework identifies the mix of generic therapeutic competences and EMDR-specific competences that practitioners must be able to demonstrate. A core professional mental health training is a prerequisite for entry into EMDR foundation training. This is in line with the training and background of EMDR therapists employed in the clinical trials that have demonstrated the efficacy of EMDR therapy and is consonant with the accreditation standards of EMDR Association Europe.
Supervision
Supervision is critical to maintaining fidelity to the EMDR model and to assure its effective and safe delivery. EMDR therapists should be supervised by individuals with sufficient training in, and experience of, EMDR, and services will need to ensure that supervisors meet these criteria. Used in conjunction with the competence framework for supervision, the Framework is potentially a useful tool to improve the quality of supervision of EMDR. It does this by focusing the task of supervision on a set of competences that are known to be associated with the delivery of effective treatments. Supervision commonly has two aims – to improve outcomes for clients and to improve the performance of practitioners. The Framework will support both, through:
· providing a structure by which to identify the key components of effective practice.
· allowing for the identification and remediation of suboptimal performance.
The Framework can achieve this through its integration into professional training programmes and through the specification for the requirements for supervision in both local commissioning and clinical governance programmes.
Commissioning services
The Framework can contribute to the effective use of healthcare resources by enabling commissioners to specify the appropriate levels and range of competences that need to be demonstrated by workers to meet identified local needs. It could also contribute to the development of more evidence-based systems for the quality monitoring of commissioned services by setting out a framework for competences that is shared by both commissioners and providers, and which services could be expected to adhere to.
Service organisation – the management and delivery of services
The Framework represents a set of competences that (wherever possible) are evidence-based, and it aims to describe best practice for the activities that individuals and teams should follow to deliver interventions. Although further work is required on the competences’ utility and on associated methods of measurement, they should enable:
· the identification of the key EMDR competences that a practitioner needs.
· the likely training and supervision competences of people managing and delivering services.
Clinical governance
Effective monitoring of the quality of services provided is essential if service users are to be assured of optimum benefit. Monitoring the quality and outcomes of interventions is a key clinical governance activity and the Framework allows providers to ensure that EMDR interventions are provided at the level of competence that is most likely to bring real benefit by allowing for an objective assessment of clinicians’ performance.
Concluding remarks
The commissioning of an EMDR competence framework by HEE is an important step towards supporting the development of EMDR therapy within NHS services. It provides a platform for commissioning more training and supervision, and it strengthens the opportunity for more outcome research.




